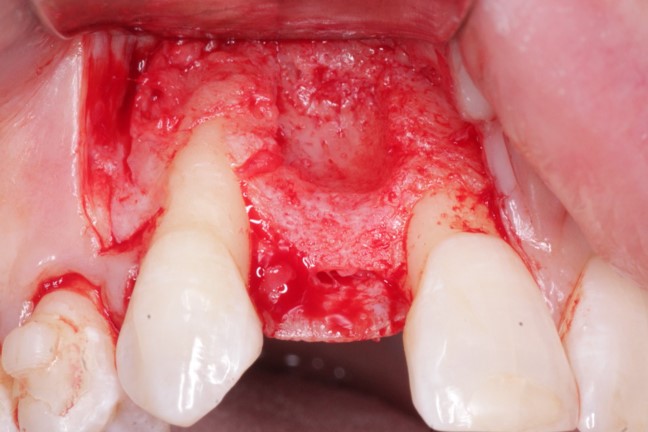
Possibly cold welded healing abutment: what to do?
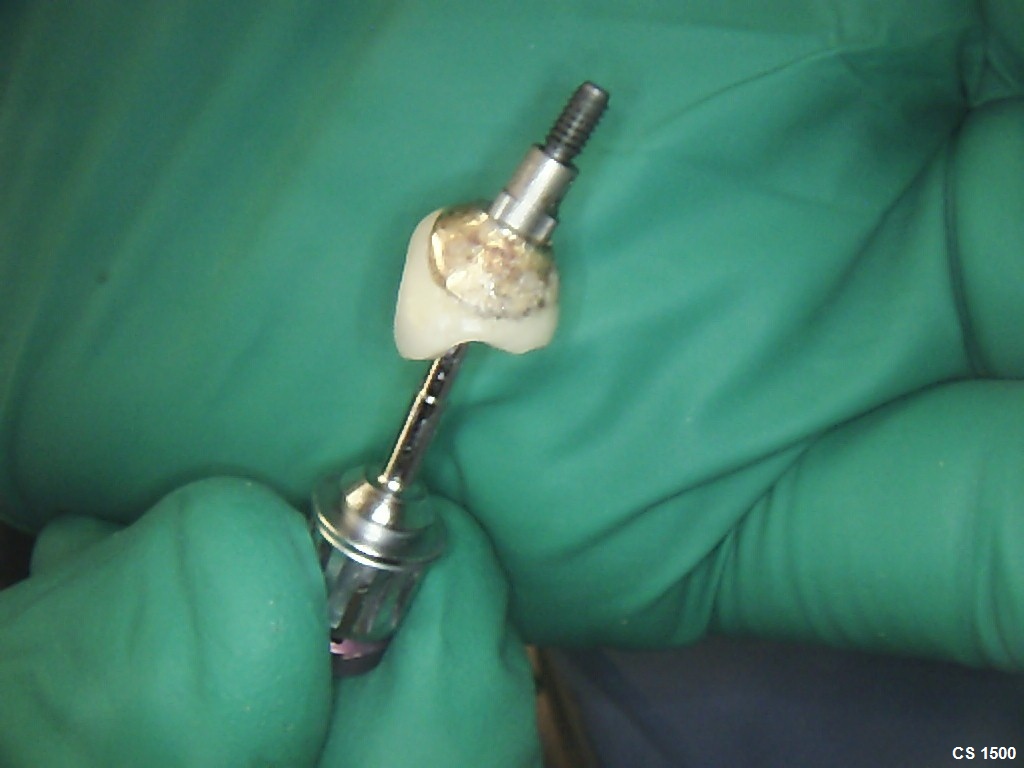
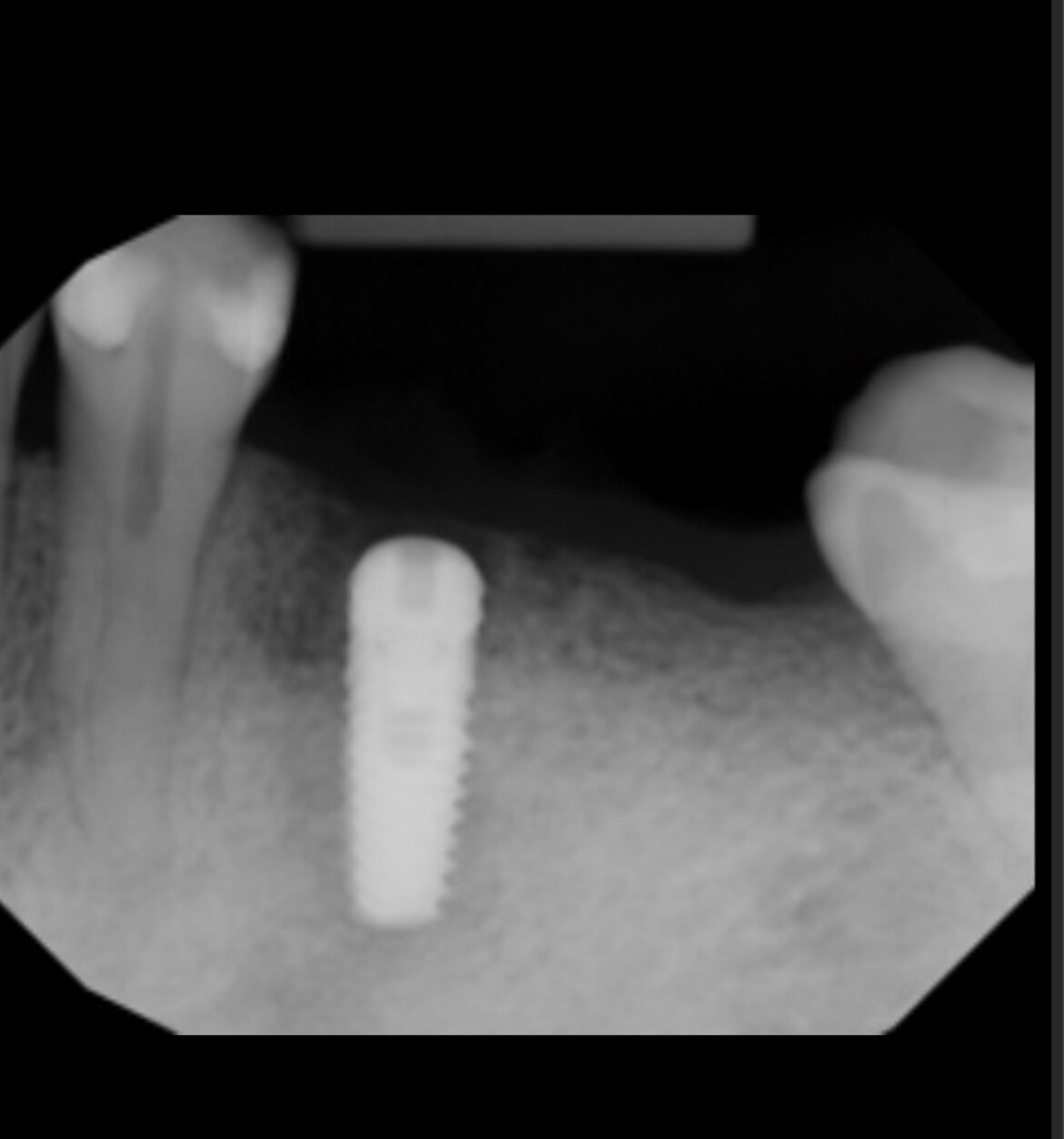
I installed a BioHorizon tapered Laser Lok 5.8 x 12mm with an internal connection in #31 site [mandibular right second molar; 47] 2 months after tooth extraction and placed a direct healing abutment. The post-op was uneventful and it seemed to heal well. After 2 months, I removed the healing abutment and placed an impression coping for pickup impression and afterward replaced the healing abutment. When the patient was recalled for crown insertion, I could not remove the healing abutment. I tried using a torque ratchet and then a machine driver with 70 N anti-torque but the healing abutment would not budge. What can I do to remove the healing abutment?

29 Comments on Possibly cold welded healing abutment: what to do?
New comments are currently closed for this post.
mazen dukhan
3/2/2015
I think you need a special pliers which can holed the neck of the implant firmly ,then you can apply a higher torque in order to remove the healing abutment .I m ready to provide you with this kind of pliers freely, regards
Ethan Moulton
5/11/2016
I used theNobel implant retrieval tool (product ref 36139) today to remove a frozen healing abutment. The cost for the nobel part is about 50-60$,
The straumann scs driver stripped when trying to remove the healing abutment, hence the need to use this tool. I was able to remove the frozen (not cross threaded) healing cap after drilling a hole in the top of the healing abutment to make space to engage the tool.
It can be used to remove stuck healing abutments or failed implants *I have used with multiple brands of implants with great success.
The groove/thread pattern on the nobel tool is a thin, narrowly spaced thread with fine grooves. They really work. First experience with it was removing a 6 x 16 tapered nobel. After trying both the neo-biotech and the Bti kit with no success.
I consider it one of the best values in implant dentistry. Get one and some cut off disks to have on hand. You will be glad you have them and at minimal cost. ***You need the gold adapter for your nobel ratchet to use the tool.***
AAslamOMS
3/2/2015
@mazen dukhan. Thank you for the offer but this is a submerged, bone level implant. How do we hold the neck of the implant plus the hex screw slot seems to have slipped now.
CRS
3/3/2015
What is making me nervous is the timing on all this. At eight weeks post op the implant is still osteo integrating and bone is remodeling. I would have waited at least 12-16 weeks post placement especially since the implant was placed in a eight week still healing extraction site. There are two possibilities here, a stripping of the healing head screw, I don't think the torque is enough to truly "cold weld" or the implant is not fully integrated so the reverse torque is not a good thing. I think the pliers suggestion will allow you to pull the implant out also. If you are an Oral Surgeon are you going to restore this implant? What will tell is over the next few weeks if the implant demonstrates bone loss on the X-rays and becomes loose. If so remove and start over allowing the ideal healing parameters. Good Luck keep us posted.
mazen dukhan
3/3/2015
when i suggest the pliers i mean this is too special for this case it has two sharp edges formed to hold cylindrical body which can holed the implant neck and embraces the healing screw inside without any contact with ,
Peter Fairbairn
3/3/2015
Happened to me and needed over 120 Ncm reverse torque which removed the Implant ......... sadly and then even after removing it using mole grips to hold it it required about 220 to remove the healing cap ..
Life goes on
AAslamOMS
3/3/2015
I suppose CRS is the Oral Surgeon here so I always look forward to hear his opinion on this, and Peter Fairbairn generally has a fairly pragmatic opinion about everything. Well, my policy is generally to wait for 8 weeks in the mandible and 12 weeks in the maxilla; add one or two more months if it is grafted. At site opening, there was good quality bone that I encountered, and had to use tap drill to ensure complete insertion of the implant without too much force. The healing was uneventful. The total wait post implant placement was exactly 9 and a half weeks. I took x rays, verified good clinical healing and then the restorative dentist came in who did a pickup impression coping. He had the healing abutment placed back, and the next time I heard from him was a worrying voice that the healing abutment is not getting off. I went as the maverick surgeon, and soon humbled when despite using the 30 N Biohorizons torque wrench, and then the 70 N anti torque on our implant motor, the abutment wouldn't just budge, and finally the hex screw slot slipped. The patient being an Engineering guy himself realized, and asked about options and I said I will research over the weekend and get back. People have suggested 1. ice application and then trying, 2. a straight slot to engage the regular home driver, 3. using an ultrasonic topic to go around the abutment, 4. Prepare the abutment to put the crown directly, 5. drill a through-and-through hole into the screw where it would somehow fracture and give way. Patient though understanding enough, does not think implant removal would be an option since he will be traveling overseas in a month and half time. CRS do you think, this excessive anti torque application might have started a bone resorption at the crest that we will realize later? @Mazen Dukhan; can I see a picture of your instrument; it will be very interesting to see. If you can post it to the Osseonews admin who can then forward it to me? Thanks.
CRS
3/3/2015
Yep, only time will tell. Read Peter's post more pragmatic. I try to be very light handed with the healing heads and screws on my implant drill the insertion torque is 15Ncm. These are tiny screws which are easily stripped. Same feel as filing a root canal. I would suggest lengthening your healing time, your policy is not helpful. When I undercover an implant and the screw is not engaging the first thing I think of is that the implant is not fully integrated. An implant that can't be restored for whatever reason is no good. I also remove or at least loosen the fixture mounts when I place implants so that the implant is not disturbed by removing a mount. I don't release the patient for minimum 12weeks mandible and 16 weeks maxilla to the restoring dentist. Another simple trick I also loosen the healing screw or abutment before I release the patient so I know it is removable. Once the patient leaves my office I have relinquished control to the other professional. Perhaps someone will post how to drill a slot for the screw or how to drill thru it then the screw will have to removed also. Someone may have torqued this abutment too tight, it happens.
mazen dukhan
3/3/2015
you can check the pics at the osseonews faceboook page.
Charles Schlesinger
3/3/2015
Try this: Put a hex driver into the healing abutment with a torque or ratchet wrench. Then use an instrument like a small mallet or the back of an elevator and give the wrench a sharp tap in the counterclockwise direction.
This will usually break the seal and free up the healing abutment. This is the safest way to do it since the force is high, but the duration is instantaneous. Much better then sustained high forces.
Good luck,
Chuck
James Talons
3/3/2015
Dr. Dukhan's primary language (I am assuming) is not english---so I am going to help with the technical part of posting the very elegant design of his device. Its on his facebook page as he mentioned---all you have to do is click on his name and scroll down--you will see the patent, and a few miscellaneous photos--and then the submitted drawing of the device he designed (to the patent office). OR--this link-which will take you to the same place.
nailesh gandhi
3/3/2015
I endorse view by Chuck. Tapping is the safest solution to unscrew. In my experience it has proved.
Raul Mena
3/3/2015
It is almost impossible for a Biohorizon abutment to cold weld to the implant, so the reason that the abutment is difficult to remove is because, overtightening of the abutment, cross threading of parts not properly matching.
Placing the cavitron over the healing abutment and then trying to unscrew it may be one of the options. Applying more force may be another solution.
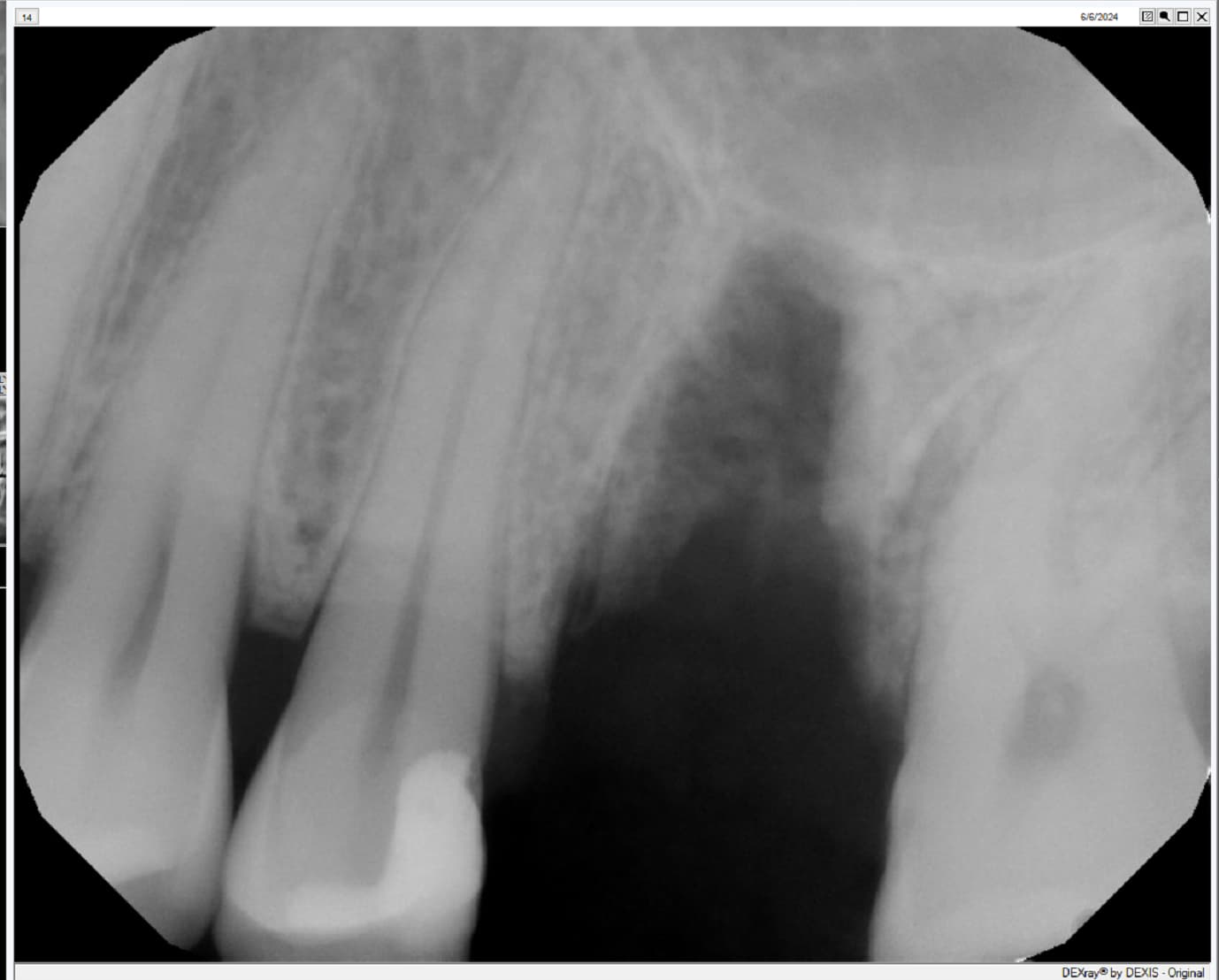
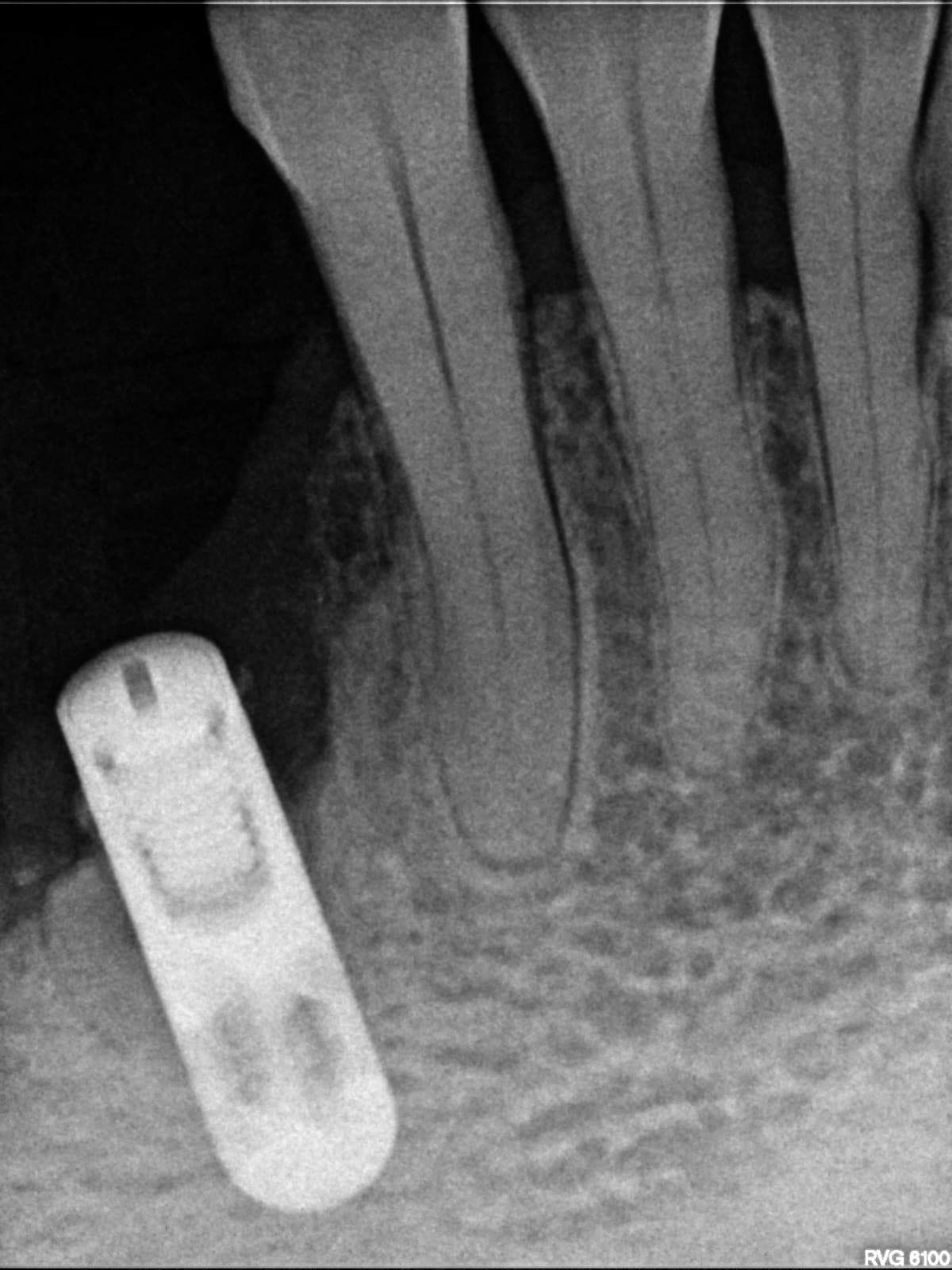
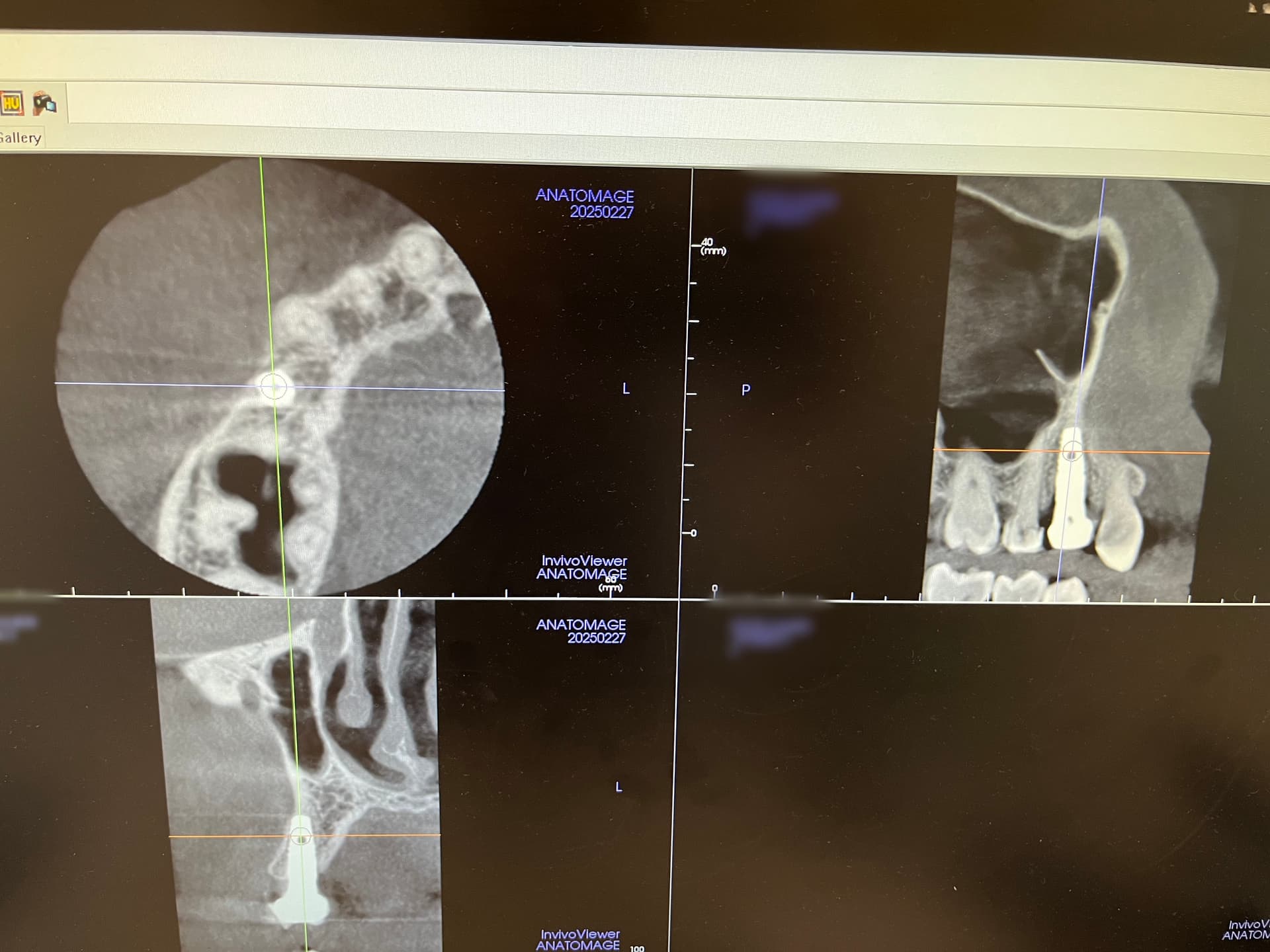
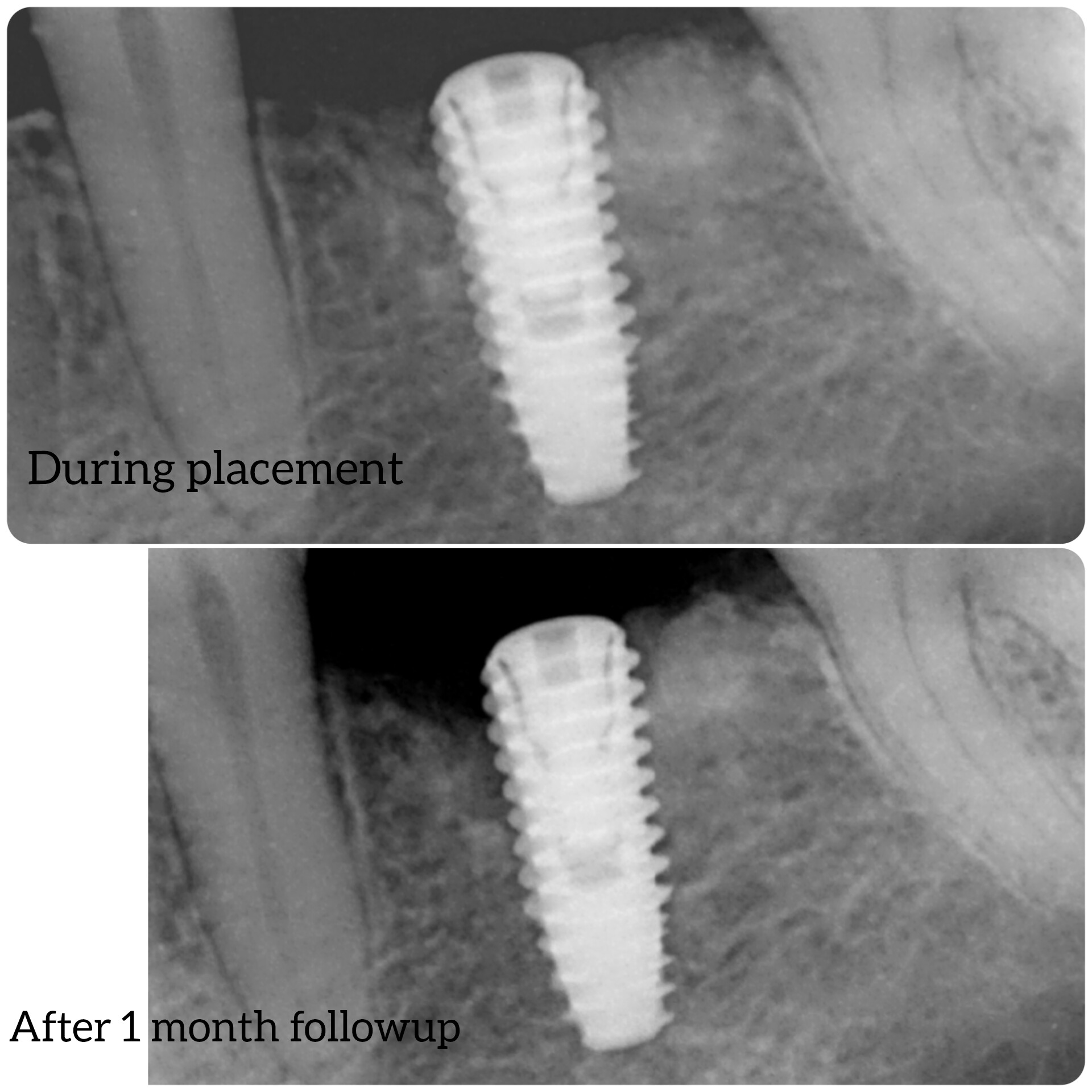
The radiograph shows bone loss at the crest, unless it is burnout of the radiograph.
I would be also concern of the periapical radiolusency at the mesio buccal root of # 30.
Raul
John Manuel, DDS
3/4/2015
In general, a cold welded connection is released by a combination of moderate rotational force in conjunction with a "withdrawing" sharp tapping force. Not necessarily a strong withdrawing force.
I am assuming you have the screw removed and that you are referring to the abutment's having a cold welded connection.
Rotational force alone won't release a cold welded connection. That's why it's used on aircraft engines and ship's propellers.
Dennis Flanagan DDS MSc
3/4/2015
There is research that shows a cold weld is not a real occurrence. I agree that it is probably a cross threading. Dennis
Nicholas Ritchey
3/4/2015
I am the Prosthetic Product Manager for BioHorizons. I would be happy to help you troubleshoot this situation. Please contact me at your earliest convenience.
BioHorizons USA
1-888-246-8338
AAslamOMS
3/4/2015
@ Nick Ritchie; dropped an email last friday; there has been no response. Just tried calling the number you have given twice, and after really long waiting, couldn't get to speak to anyone, including the operator!!
@ Raul Mena; the relative less density distal to the implant is traces of the socket, which takes typically 6 months to become radiologically indistinguishable. How overtightening one can possibly do with fingers?
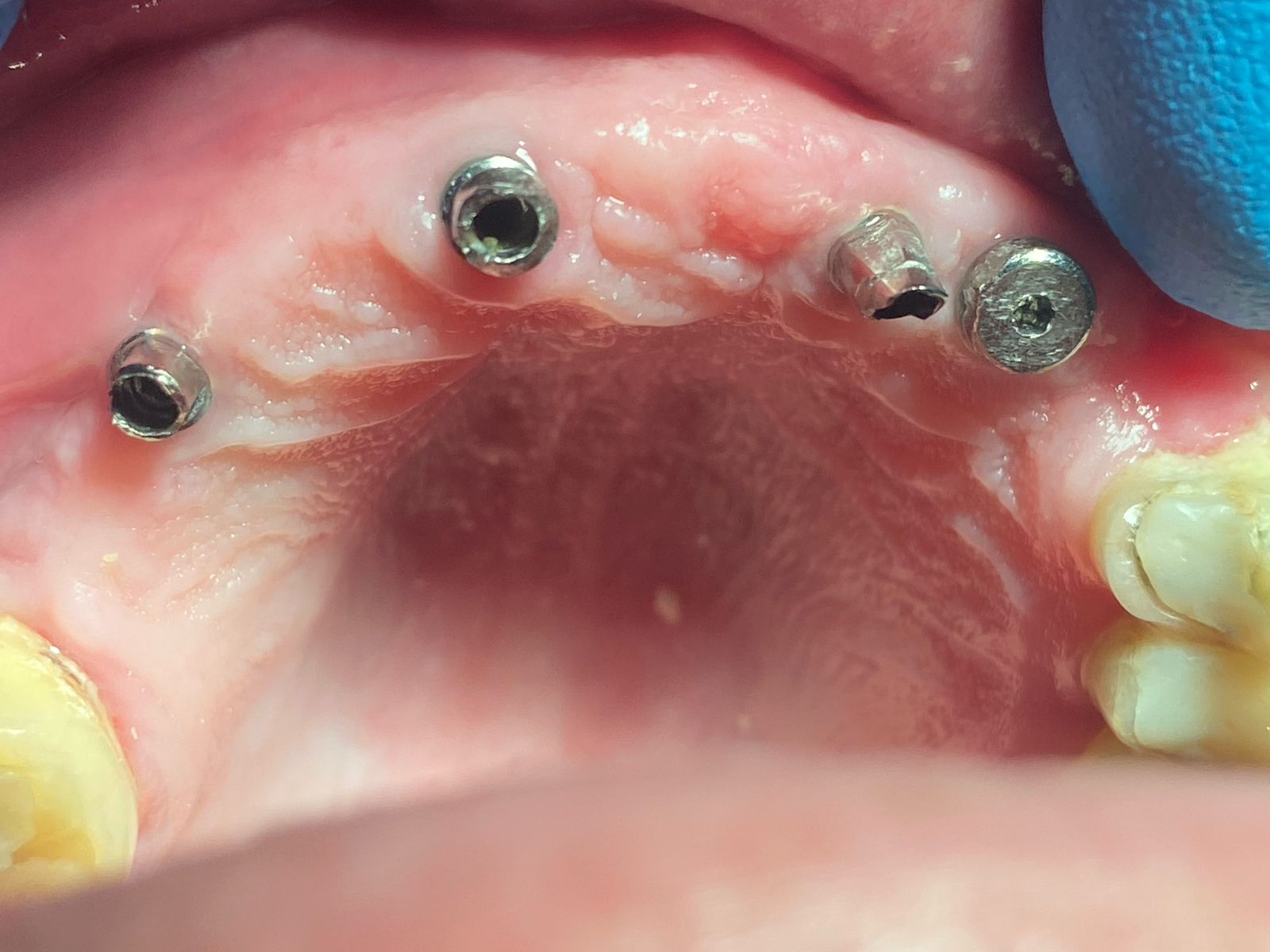
Is everyone alluding to the fact that we use a fractured screw removal kit? The hex screw slot has slipped now. Will use a scaler tip anyway to impart some vibration.
Matt Helm, DMD
3/4/2015
@AAslamOMS: The short answer here? Choose your own option #4 AAslamOMS! It is the best, and easiest solution to your dillema, by far (to solve the problem for the patient, as well as for yourself, from a patient management standpoint). And here is why and a few other points to consider:
Simply prep the healing abutment and crown it. That was option #4 in your list of possiblities. Make sure you don't over-taper! Prep the healing abutment with just a minimal taper to enhance the mechanical retention of the crown. If the healing abutment is too short and you're concerned you may not have sufficient retention, you can obtain additional retention and stability by also prepping out the hex-hole in the healing cap's head slightly conically toward the surface (as if to receive a cast post) and have the metal coping of the final crown cast with an integral internal post, like in a Richmond crown. The hex is already stripped anyway, you cannot do it any more harm. If the resulting abutment (the prepared healing cap) is too short, and you still have retention/stability concerns, cement the crown with a self-cure resin, With weak retention the crown will still be easily removable for maintenance. You should also add a couple of longitudinal (vertical) grooves in your preparation (of the healing cap) to also add a bit more mechanical retention and anti-rotation to the crown. You may think those vertical grooves are insignificant, but every little bit helps. (Remember that it is the sum of the details that create the final result.) Take the impression like you would for any other crown prep. Make sure the emergence profile of the final crown has no height of contour right at the gingiva, which would retain food and traumatize the gingiva, possibly causing slow coronal bone loss or peri-implantitis over time. This detail is even more important if you are unable to create any sort of chamfer or shoulder at the gingival margin of the preparation. It is imperative that the final crown should taper smoothly coronally from the free gingival margin. The placement of the natural (anatomical) buccal and lingual heights of contour to direct the food bolus away from the gingiva is also imperative, but it must not be done in such a way as to cause an excessive undercut in the gigival 1/3 of the crown.
Considering the patient's short travelling time frame, this is your best, most efficient, and least head-ache prone solution, Considering the implant is still fresh and, as per the x-ray, bone has not fully healed around it's head, specially in the distal, all other solutions would disturb the implant excessively. Applying ultrasound may work but it may also damage implant stability long term. I see it as too risky, specially in such fresh implants. Likewise the solution with the counter-holding pliers involves applying a gread deal of force on the implant, which is also very risky. Even with the special pliers that would counter-hold the implant as you try to unscrew the frozen healing cap, it is humanly impossible to avoid applying excessive force to that implant, in one direction or another at some point during the procedure. Do yourself the favor and prep the healing cap for a crown, and save yourself AND the patient the unnecessary additional sweat. Two months is way too early to disturb this implant in any other way, which is only about 75% in solid bone, at best, and only 50% on the distal. I would not have restored prior to 12 weeks. I have seen this situation before, and have witnessed other's attempts which resulted in disaster (removal of the implant or its failure in just a few months time).
I personally have solved it as described above, and it was by far the best and least risky solution of all. Best of all, it worked out very well. Remember that one of our mottos is to do no harm. Preparing the healing abutment for a crown does no harm to the implant, or the patient.
Raul Mena
3/4/2015
Dear AAslamOMS
How about the radiolusency at the apex of # 30 mesial root?
Raul
AAslamOMS
3/5/2015
@Raul Mena; the 46 is asymptomatic and didn't notice the radiolucency before in other radiographs. Will investigate it though.
@Matt Helm; thank you very much for a very detailed explanation and least risky solution suggestion.
Matt Helm, DMD
3/5/2015
@AAslamOMS: You are quite welcome! Glad you liked it. It is indeed the least risky, easiest, and kindest solution by far. I am always for erring on the side of kindness.
I also omitted to mention that if the implant collar (or even any of the implant threads) protrudes from the gingiva, you can ALSO gain additional crown length by preparing the part that protrudes with a diamond and copious water cooling. You don't need to prep much, just enough to elimnate the implant's threads (if any are showing) and create a taper. Any mm you gain in the length of this crown will aid retention and stability. You have nothing to lose if you prep the collar (or even part of the implant) because since the healing cap is so frozen you'll never be able to place a proper abutment on this implant anyway. Use the tricks I described -- the post prep in the healing cap and vertical prep grooves -- to add retention and you'll be just fine!
Had you tried any of the other alternatives you would most certainly jeopardize the implant, maybe even yanked it out, because even though it may have looked submerged clinically at the time of placement, radiographically it is not. I especially don't like the distal, where radiographically only 50% of the implant is in solid bone. That means bone is a long way off from truly forming, specially on the distal, and that's IF it will ever fully form all the way up to the implant collar..I especially dislike the counter-plier solution as being too traumatic and risky. Once an implant is placed, it should be forced or torqued as little as possible.
I don't know how this healing cap was placed or who placed it, but as a point of safety, I always prefer placing healing caps and abutments BY HAND. You can never go wrong with your finger feel. Using the handpeice can cause cross-threading, which is what I believe happened in this case. Good luck and let me know how it works out!
CRS
3/6/2015
Very good advice let the patient decide if restoring on the healing head while not ideal vs removing and starting over. I still would wait until enough time passes for osteointegration. By the way I think it is nobel of you to try and fix this but not profitable if you did not lock this on. Perhaps shared expense of retreatment with dds. Personally I would remove and start over so that it is right so that the case will not come back to haunt you. I have found that these situations rarely result in an enhanced referral relationship, the dentist usually goes elsewhere vs facing the problem and learning from it. Whatever you do informed consent is critical this is not dental school where you can wing it with creative solutions.good luck I do feel however that Dr Helm's solution is a good option but have the restoring dentist assume the responsibility if you recommend removal. Group consensus dentist patient and surgeon.
Matt Helm, DMD
3/7/2015
@CRS: Thanks CRS. Glad you liked it also. I do agree that more time for osteo-integration should be given. Like you, I also wait 12 weeks in the mandible and 24 weeks in the maxilla.
I also agree that the dds needs to own at least part of this. From AAslamOMS's description of the events of that fateful visit when the impression was taken, it sounds like this healing cap became frozen right after the dds placed it back after taking the impression. Since the incident was instantaneous (as opposed to not being able to remove the healing cap from one visit to another) odds are that this is indeed a cross-threading situation and that it was the dds who cross-threaded it. True cold-welded has not really been documented. And while I'm not looking to place blame for blame's sake, I think a bit of responsibility on the part of the dds (not to mention a learning experience) is warranted. Let him learn to thread everything by hand. Haste makes waste, as the old addage goes.
From a pure patient management standpoint however, I personally think most patients would prefer to avoid removal and re-insertion of the implant, given the choice. Aside from the additional trauma, there is also the additional time to final restoration. No one likes that, specially not this patient who has a tight travel time-frame. If the patient is presented am alternative solution to solve the problem with minimal fuss, while informed consent is also given, most patients would opt for the easier solution -- mine. It is all well and good to prefer to have an ideal outcome (by removal and reinsertion) but sometimes that can cause more harm, specially in the Dr-patient relationship. Conversely, a patient in this predicament (and an engineer no-less, like this patient is) will appreciate the effort and the ingenuity of solving the problem without the added time and trauma of replacing the implant, thereby preserving (and possibly even enhancing) the Dr-patient relationship. Engineers always appreciate creative work-arounds. If AAslamOMS solves this with minimal grief and time to the patient he will come accross as "a hero" and, the patient may even refer to him more readily. As for this coming back to haunt, hardly. Preparing and crowning the healing cap should have almost an identical final functional result (as a proper abutment would) with very few drawbacks, if the crown is properly done, specially gingivally. Attention to detail is key. And of course rigorous follow up.
Group consensus is indeed key and, patient approval is paramount, but oftentimes it is up to us to educate and giude the patient in the right direction.
AAslamOMS
3/10/2015
Thank you everyone; got lucky today, and it came out quite easily today after a lapse of about ten days. Had seriously started to think about asking the restorative colleague to do a healing abutment preparation to directly receive a crown. However, thought should give it one serious try. Tried the regular scaler (Cavitron) gently in an anti clockwise direction twice for about 4-5 minutes each. Then the restorative dentist had the slot through the healing abutment deepened adequately, and when the flat head home use screw driver was inserted, it came out with almost no force. Guess the scaler had done the trick already and it just needed a little bypass mechanism to derotate through a regular screw driver. Have put the picture on the facebook picture here at
@ Raul Mena; the adjacent first molar tip is all clear. No endo/perio on x ray.
CRS
3/13/2015
Hallelujah! Now go and sin no more⛪ï¸
Matt Helm, DMD
3/14/2015
Well, glad you got it out. You got lucky. It may have been the scaler trick, but I tend to think it was a combination of a couple of things. Maybe letting it sit a week simply loosened it due to a slight metal contraction and, maybe all the previous attempts at loosening it also played a role. And sometimes, when you let something sit and come back to it later, you take a bit of a different approach, albeit subconsciously. Regardless, all's well that ends well. Congrats! Remember my crowning the healing cap trick for next time. I have seen this happen and the healing cap could not be removed for anything in the world. So while I don't widh it on you, it's always a possiblity.
E Chan
3/23/2015
What r the chances of the implant re-osseointegrated after it is loosened during healing cap removal and implant immediately placed back in the socket? a colleague had encountered similar situation n told me that he had loosened the implant during healing cap removal but implant was quickly placed back. he gave it time n eventually the implant osseointegrated, n he restored the tooth.
Olof heden
12/16/2015
From Senior
Wien you have problem to lose healing caps. Spray coldspray on a cottonpellet and hold it on The CAP for 5 seconds. Now you can unscrew the CAP.
Regards Olle
MAS
6/30/2017
it has happened to many. I have tried simple technique of tapping the healing abutment with back to mirror handle (exactly when bottle cape does not open one tape it all around gently with spoon before opening). It breaks the cold weld bond. Generally it works.